Imagine a hug. A really tight, painful hug that seems to last forever and your body is doing it all by itself. This is one symptom of multiple sclerosis (MS) called an MS hug. 2 million people in the US live with MS. There is no cure, therapies are often ineffective, and the disease just gets worse over time. A vaccine for MS would be revolutionary, and it’s on the horizon. The same mRNA technology that got you your covid shot could get me my MS shot (at least, a girl can dream).
What is MS?
The immune system is designed to protect your body from foreign invaders like bacteria or viruses. Autoimmune diseases occur when rogue immune cells attack your healthy body instead of foreign invaders. MS is a type of autoimmune disease where these rogue immune cells attack the brain and spinal cord causing cognitive impairment (problems with memory, language, and thinking) and motor disability (partial or total loss of function of a body part).
Most people with MS are diagnosed between 20 and 40 years old, typically after a patient experiences symptoms of the disease. Because MS is a chronic disease, disabilities accumulate and worsen over time. Patients are treated with broad immunosuppressants designed to suppress whole branches of the immune system because technology has not yet advanced to target just those rogue cells. This means that people with MS live without their full immune systems, at increased risk of acquiring infections – while dealing with current disabilities and the potential onset of more MS symptoms.
What’s happening on a cellular level?
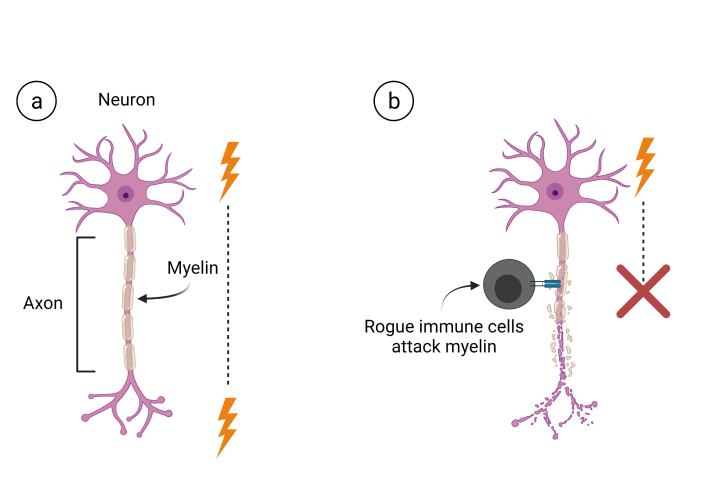
The brain and spinal cord make up the central nervous system (CNS). The CNS is a network of billions of cells called neurons that carry electrical messages between the brain and the body. Neurons are connected to each other by axons which are long extensions that come off the neuron like a power cord off a vacuum. Neurons send electrical messages that travel along the axon to communicate to other neurons like how an electrical signal from the wall socket runs along the power cord to a vacuum motor. Like any electrical cord, this connection between neurons needs to be insulated to speed up and protect the electrical signal. On your vacuum, the metal wires that actually carry the electricity are insulated by a plastic coating on the outside of the power cord. In the CNS, this insulation is a fatty material called myelin (Figure 1a). The longer and thicker the myelin is, the faster those electrical signals travel along the axon.
In MS, rogue immune cells mistakenly recognize myelin as harmful and attack it. This breaks down myelin and slows or interrupts the electrical signal that axon was supposed to conduct (Figure 1b). This disrupted electrical signal is what presents as disability (ranging from inability to move a leg to inability to find the right word).
The million dollar question – can we stop these rogue immune cells?
In an exciting new discovery from Christina Krienke and colleagues working at TRON* in collaboration with BioNTech, a similar mRNA vaccine technology playing a pivotal role in fighting the COVID-19 pandemic is now being applied to MS. They created an MS vaccine that works by defending myelin from rogue immune cells. Their vaccine harnesses the regulatory side of the immune system which is designed to “catch” rogue cells before they’re released into the body’s circulation. Important cells in this regulatory system called Treg cells patrol the body to make sure healthy tissue is not attacked. This vaccine teaches Treg cells that myelin is safe and should be protected.
How does it work?

The vaccine uses mRNA which acts as a blueprint cells use to make proteins or shorter segments of proteins called peptides. In this case, the mRNA codes for a peptide segment of myelin protein called Myelin Oligodendrocyte Glycoprotein, or MOG peptide. Once injected, the MOG mRNA is transformed by healthy cells into MOG peptide which is then presented on a cell’s surface. Since the cell presenting MOG is healthy, Treg cells interacting with it associate MOG with healthy cells, teaching the Treg cells that MOG is safe and should not be attacked (Figure 2). Treg cells carry this lesson with them wherever they go in the body, including the CNS where they might see rogue immune cells attacking myelin. Since myelin is made of MOG, and the Treg cells now know that MOG is safe, they will intervene and stop rogue cells from attacking myelin (Figure 3).
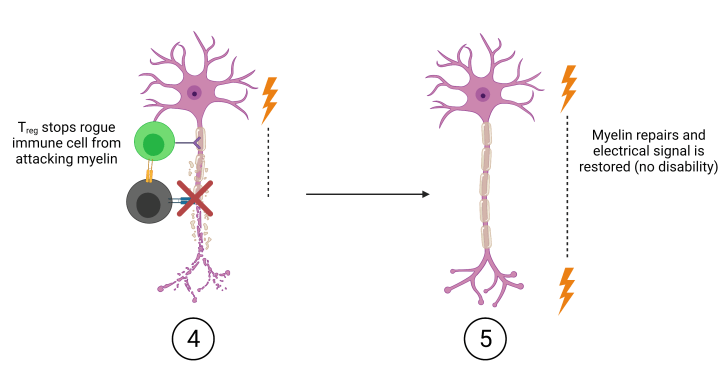
You may be thinking that just introducing a new regulatory cell doesn’t get rid of the myelin-targeting immune cells that are already in circulation. But research shows that Treg cells are more effective at preventing disease than deleting those rogue immune cells entirely. In other words, it’s better to send a scout to wave their arms and call off the troops than to remove the troops entirely.
Once myelin is no longer under attack, healthy CNS cells produce new myelin to repair the wrapping around the axon. If the axon fully remyelinates, neurons can again fire complete electrical signals and disabilities disappear (Figure 3).
What’s the data?
Krienke et al. have so far tested the vaccine in mice using a commonly used animal model for MS called experimental autoimmune encephalomyelitis, or EAE. Their paper published in January 2021 came back with remarkable results. They found that the vaccine not only prevented further disease progression, but it also fully restored all motor function the mice lost during the disease! If these trends continue through human clinical trials, this MS vaccine has the potential to change millions of lives, including the life of this author.
This article summarizes work from: Christina Krienke et al., “A Noninflammatory MRNA Vaccine for Treatment of Experimental Autoimmune Encephalomyelitis,” Science 371, no. 6525 (January 8, 2021): 145–53, https://doi.org/10.1126/science.aay3638.
* Translational Oncology at the University Medical Center of the Johannes Gutenberg University
All figures created with BioRender