One of the main functions of our immune system is to protect ourselves from strange agents. Pregnancy is a physiological state in which foreign cells “invade” the maternal tissue. To avoid the elimination of this “invasion” and complete the process of formation, growth, and birth of the progeny, the maternal immune system must be regulated and dynamically adjust responses to the fetus. The immune system, therefore, must be robust and responsive in order to both tolerate the fetus and protect the mother and fetus during pregnancy.
Implantation is the process in which trophoblast cells attach and invade the uterus surface (decidua) forming the placenta. Trophoblasts are cells of the fecundated egg that will nourish the fetus. In order to be successful, the implantation process needs an anti-inflammatory environment in the uterus with maternal immune system suppression to allow the fetus to develop and grow. Anti-inflammatory cytokines and cells, such as regulatory T cells (Tregs), macrophages, and uterine/decidual Natural Killer cells, are responsible for this important task. Understanding the function of these cells during pregnancy could help to decrease the risk of pregnancy complications, such as preeclampsia, which is a disorder with placental and endothelial (layer of cells that forms the blood vessels) dysfunction. Preeclampsia leads to hypertension and organ damage and alters otherwise healthy pregnancies, potentially causing severe complications to the newborn and the mother.
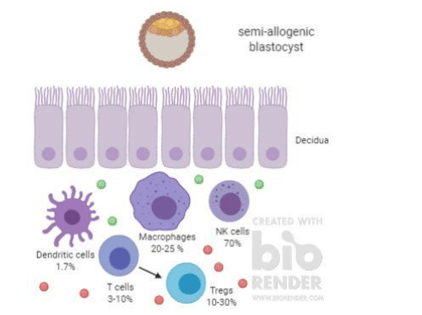
Figure 1. The microenvironment of the decidua during pregnancy with immune cell proportions. Green and red dots represent anti-inflammatory cytokines and chemokines, respectively. Created with BioRender.
Let’s talk about the players
Trophoblast cells are the first contact of the fecundated egg within the maternal uterus and can generate a more receptive pregnancy environment, (i.e. an anti-inflammatory environment (presence of macrophages type 2, Tregs, uterine NKs)). Trophoblasts can induce a less toxic and more tolerant type of Natural Killer Cells (NKs) as well as facilitate the differentiation of T cells to Tregs. Trophoblasts themselves give signals to facilitate their acceptance by immune cells. In addition, they can express receptors called NLR (NOD-like receptors) that recognise pathogens and other damaging agents, (free radicals, dying cells). All these functions are shared by immune cells, making trophoblast cells very versatile and relevant for the success of the pregnancy.
NKs protect mother and fetus from pathogens during pregnancy, and uterine/decidual NKs (uNKs) are crucial for the trophoblast invasion and blood irrigation of the uterus. Interestingly, uNKs can “learn” from the pregnancy experience. During the first pregnancy, uNK populations that detect the trophoblast are found in lower proportions in comparison with subsequent pregnancies. These uNKs help the uterus environment to “remember” the trophoblast and respond to its implantation more easily the next time around.
The main functions of Tregs in the body are to avoid reaction to self-antigens and non-dangerous foreign antigens and to limit excessive inflammatory response, inducing tolerance. During every ovulation, Tregs are recruited to the uterus in response to estrogens, prepared for a potential pregnancy. Their numbers increase in the endometrium during egg implantation and reach their peak from early gestation to mid-term pregnancy. As their name implies, Tregs mainly regulate the inflammatory function of other immune cells (such as macrophages, NKs and dendritic cells) by producing cytokines and chemokines. At the same time, other immune cells control the number of Tregs, resulting in a feedback loop. The majority of T cells in uterus will be specific to the fetus after the pregnancy, helping the implantation process in following pregnancies.
What happen if the tolerance is interrupted?
Complex interactions and communication between the fetal-maternal system and the placenta exist during pregnancy. During preeclampsia, immune regulatory mechanisms are altered. Pro-inflammatory signals increase and anti-inflammatory are reduced, increasing the probability of a fetal rejection. The dysregulation of Tregs is associated with poor trophoblast invasion and placentation and dysfunctional blood irrigation. In consequence, fetal growth is restricted and severe preeclampsia occurs with the risk of preterm labour and spontaneous abortion.
Additionally, the presence of pathogens affects the equilibrium of the immune response during pregnancy: pathogens can induce preterm births, injury, death of the fetal-placental unit, and abortions. The type of infection, the time of infection, and the degree of the maternal response changes the impact of the infection to the fetus. Maternal microbiota induce tolerance and facilitate implantation, however, it is important to note that human healthy placentas are sterile and do not contain microbiota, and the presence of microbiota is a sign of pregnancy complications.
Due to the important function of Tregs in pregnancy, accurately screening their numbers is crucial. Tregs numbers increase in healthy pregnancies: in a rat model of preeclampsia, symptoms were mitigated when Tregs from a healthy pregnant donor were transplanted. This represents an excellent potential for a therapeutic, but more research is still needed. Sophrosyne, a valuable lesson of the Greek culture and art, refers to equilibrium, and a concept of balance. Pregnancy and other biological processes require this equilibrium to be successful, and Tregs are one of the supervisors.
For more information:
- Colucci, F. The immunological code of pregnancy. Science 30 Aug 2019: Vol. 365, Issue 6456, pp. 862-863 DOI: 10.1126/science.aaw1300
- Robertson et al Front. Immunol., 21 March 2019. https://doi.org/10.3389/fimmu.2019.00478
- McDonald and McCoy, Maternal microbiota in pregnancy and early life Science. 2019 Sep 6;365(6457):984-985. doi: 10.1126/science.aay0618.
- Han et al Front Immunol. 2019 Jun 11;10:1305. doi: 10.3389/fimmu.2019.01305. eCollection 2019.
- De Goffau et al. Human placenta has no microbiome but can contain potential pathogens. Nature. 2019 Aug;572(7769):329-334. doi: 10.1038/s41586-019-1451-5. Epub 2019 Jul 31.
- https://www.nature.com/collections/nyhmtlnwwq
Mariana Pacheco currently is a Post-doctoral researcher at Biocev (Biotechnology and Biomedicine Centre of the Academy of Sciences and Charles University in Vestec, Czech Republic) studying molecular mechanisms in lymphoma biology.